Redefining Self: Patient’s Decision Making About Treatment for Multiple Sclerosis
Why is this important to me?
Several treatments are available for treating the relapsing-remitting form of MS, and beginning treatment as soon as possible after an MS diagnosis is often recommended. The decision to begin potentially life-long treatment is complex and personal. Treatments do not cure MS, and healthcare professionals cannot predict with certainty if someone will benefit from a particular choice of therapy. The timing of when to begin treatment must often be considered if a competing goal such as having a baby is involved. Some patients may feel poorly equipped to make a decision about beginning treatment.
What is the objective of this study?
Nine people with MS participated in interviews regarding their experience with making a decision about beginning treatment for MS. The main conclusion that emerged from the study is that patients needed to redefine their sense of self. They needed to accept their “new normal” of being someone with MS and could not make treatment decisions until this was accomplished. Treatment choices were made after reflecting on their social, emotional, and physical self-image, their life and career goals, and their current and anticipated quality of life. Six elements of this core theme of accepting a new normal were identified:
- Weighing and deciding what is important: Decisions about one variable (such as having a baby for example) affected others (such as managing symptoms).
- Acknowledging the illness as part of oneself: The patients needed to accept that they have MS.
- Coming to terms: Patients struggled with fear and uncertainty about MS and its treatment options and outcomes.
- Seeking credible resources: Seeking the experience of others living with MS is especially helpful.
- Evaluating symptoms and quality of life: The patient’s perception about the possibility of MS-related disability was very important in decision making. Some patients preferred a proactive approach to treatment, and others considered treatment only when symptoms or quality of life worsened. However, symptoms alone did not affect a decision to begin treatment, but rather the impact of symptoms on their quality of life.
- Managing roles and involvement of family: Family members provided support, encouragement, and interpretation of information, and sometimes served as a member of a team of decision makers.
In addition to the above six elements of accepting their new sense of self, participants with MS reported several other perceptions, beliefs, and issues that were important when making treatment decisions. These factors needed to be considered:
- Examining their MS in a broader social context in terms of what others will see as “normal”.
- Previous experience with other illnesses and treatments: For example, injections for diabetes are often perceived as acceptable, which helped one participant perceive injections for MS as acceptable.
- The amount of time since the MS diagnosis was important, as many participants were overwhelmed and unable to make decisions about treatment soon after diagnosis. Thus, many patients will need time to make sense of MS and what it will mean in their life before they can make a decision about treatment.
- Participants valued a good fit with their physician in terms of styles of making decisions about treatment.
- All participants wanted accurate information, which was obtained from multiple sources. However, sometimes too much information was overwhelming. In general, decision making is not a linear process, but requires repeated consideration of information. Because new treatments and recommendations are continually emerging, patients will often have to consider new information and perhaps revise an earlier decision.
- Above all, patients should not hesitate to discuss their treatment decisions with their healthcare professional.
How did the authors study this issue?
The authors enrolled nine patients with relapsing-remitting MS (7 females). Participants were interviewed and encouraged to give open-ended responses and explanations. Patients talked about treatment decisions they had made in the past and decisions they were currently facing. Interviews were audio recorded, and the study authors reviewed the interviews and extracted themes related to the decision-making process.
Original Article
Redefining Self: Patients’ Decision Making About Treatment for Multiple Sclerosis
Journal of Neuroscience Nursing
Diane Lowden, Virginia Lee, Judith A. Ritchie
The treatment of multiple sclerosis (MS) has become possible with the advent of disease-modifying therapies, but little is known about patients’ experiences when faced with a complex array of treatment options. The purpose of this phenomenological study was to explore the lived experience of making a first decision about treatment with disease-modifying therapies for relapsing-remitting MS. Nine participants shared their perspectives on negotiating the decision to accept, refuse, or delay treatment. All individuals described a core theme in which decision making about treatment was part of a process of coming to a ‘‘redefined self.’’ This core theme included reflections about self-image, quality of life, goals, and being a person with MS. Six common themes supporting this core theme were (a) weighing and deciding what’s important, (b) acknowledging the illness as part of oneself, (c) playing the mental game, (d) seeking credible resources, (e) evaluating symptoms and fit with quality of life, and (f) managing the roles and involvement of family. The findings of this study provide a greater understanding about the experience of making a therapeutic choice for those with MS and offer insights for nurses when supporting patients faced with options about treatment.
Multiple Sclerosis (MS) is an inflammatory, demyelinating illness and the most common central nervous system disease of young adults. It is most often characterized by recurring attacks of acute neurological dysfunction followed by partial or full recovery (Gasperini & Ruggieri, 2011). Over time, there is a tendency to convert to a progressive form of the disease with fewer relapses, acceleration of disability, and accumulation of irreversible neurological deficits (Scalfari et al., 2010). Several treatments have become available for the relapsing-remitting form of MS, and early intervention is often recommended to limit future disease activity (Derwenskus, 2011).
The need to make a treatment decision can occur at any time, but patients often face decisions about disease-modifying therapies soon after the diagnosis of MS. The decision to initiate therapy is complex and personal. Not only do patients need to navigate information about the disease and its management when they may be feeling distressed and overwhelmed (Barker-Collo, Cartwright, & Read, 2006; Morgante et al., 2006), but they need to make a decision about whether to begin a therapy that may be administered throughout their lifetime. Making a choice to begin treatment can be difficult because treatment does not lead to cure and there is uncertainty as to who will benefit. There are relatively few biomarkers of treatment success, and there remains the possibility of continued disease activity. Some people consider whether to start treatment in the context of a perceived modest benefit. Patients may also need to consider the timing of when to begin treatment during an otherwise healthy life situation (Carder, Vuckovic, & Green, 2003; Thorne, Paterson, & Russell, 2003). Competing priorities such as plans to begin a family (Smeltzer, 2002) may require them to defer treatment. Given the uncertainty of benefit, patients are often asked to participate in making the actual choice of therapy; this may be a decision they do not feel equipped to make soon after receiving the diagnosis of MS (Heesen, Ko¨pke, Richter, & Kasper, 2007). Therefore, it is unclear which aspects they must negotiate before accepting or declining treatment and the extent of involvement they would like to have when making a treatment choice. To effectively help patients make a choice that is right for them, nurses need additional insights to understand the treatment decisionmaking experiences of these patients. The purpose of this study was to describe the lived experience of making a first decision about treatment with disease-modifying therapies among individuals with relapsing-remitting MS.
Literature Review
Decision Making in Chronic Illness
Within a self management approach to chronic illness, people need to be supported when making decisions about their health (Thorne, Con, McGuiness, McPherson, & Harris, 2004, Thorne et al., 2003; Wagner, 1998). One well-developed approach to decision support has included decision counseling and use of structured aids that are evidence based (Stacey, Kryworuchko, et al., 2012; O’Connor et al., 2009; Degner & Sloan, 1997). Decision aids provide a detailed, specific, and personalized focus on treatment options and values regarding possible benefits and harms of treatment and health outcomes (Stacey, Bennett, et al., 2012). Use of such aids has been found to increase patient participation in decision making, improve knowledge and realistic expectations, increase satisfaction, decrease decisional conflict, reduce the proportions of people who remain undecided, and increase the number of patients achieving decisions that are informed and consistent with their values. (Stacey, Kryworuchko, et al., 2012). Studies on decision making specific to MS have considered informed decision making, preferred and realized decision-making roles, and risk knowledge. Programs that systematically use a decision aid have found it to improve patient knowledge and care satisfaction (Heesen, Solari, Giordano, Kasper, & Ko¨pke, 2011; Solari et al., 2010). The emphasis in these studies on MS treatment decision aids is on providing information and education to patients within a shared decision-making partnership with their practitioner.
The Treatment Context in MS
Disease-modifying therapies for MS reduce the frequency and severity of relapses, decrease the number of MS lesions on magnetic resonance imaging, and may forestall the development of disability (Derwenskus, 2011). Medications are self-administered by oral, subcutaneous, or intramuscular routes of administration or given intravenously at infusion clinics (Derwenskus, 2011; Gasperini & Ruggieri, 2011). They have efficacy on a number of short-term outcome measures (Goodin et al., 2002), but patients may experience side effects and thus have difficulty adhering to their regimen (Berger, Hudmon, & Liang, 2004; Fraser, Hadjmichael, & Vollmer, 2001; Giovannoni, Southam & Waubant, 2012). In spite of the clinical efficacy demonstrated in clinical trials, individual patients can continue to experience disease activity (Markowitz, 2010). Several other parenteral and oral therapies from MS are being studied, which, if later found to be beneficial, will add to the therapeutic landscape (Saida, Eckstein, & Calabresi, 2012) and increase the complexity of the choices to be made by both practitioners and patients.
In this qualitative study, the researchers examine the decision-making experience of individuals living with MS and the ways in which this may affect treatment choices
Decision Making in MS
Practitioners often assume that a knowledge deficit exists when patients are undecided about treating their MS, although in reality, there is not always receptivity to receiving further information. Nurses working in the field of MS provide education to patients and families on different therapies and facilitate the decision-making process about whether to start a treatment, the timing of treatment initiation, and which therapy to choose. However, patients seen in clinical practice have demonstrated a wide variability in their interest to receive educational materials or even engage in a discussion about therapies, much less in using a decision aid or making a decision about treatment.
There is, therefore, a need to understand more about the decision-making experience of individuals with MS to consider the readiness of patients to engage in treatment decision making, to clarify when it might be appropriate to introduce a decision aid, and to identify the type of decision counseling that may be useful for individuals with MS related to pharmacological treatment for their illness.
Study Question
What is the experience of treatment decision making in individuals with relapsing-remitting MS?
Methods
The study design was Colaizzi’s (1978) phenomenological method. This exploratory method was chosen to provide a better understanding of the influences that impact the choices involved with treatment for MS.
A purposive sample of adult individuals was recruited from an MS program in a university teaching hospital. Participants were eligible for inclusion in the study if they were diagnosed with relapsing-remitting MS, had two relapses of MS in the past 2 years, and have an Expanded Disability Status Score of G7.0; were told by their physician that they were eligible for disease-modifying therapies and they need to make a decision about whether to begin treatment or not; made a treatment choice to accept, postpone, or decline treatment, within the last 3 months, or were currently engaged in the decision-making process; and/or were able to speak English or French.
Patients were excluded from the study if they had cognitive changes that would impair their ability to provide informed consent or to fully describe their experience of decision making, and/or did not consent to be audio-recorded.
Purposive sampling is a feature of the phenomenological study design and involves purposefully selecting cases with a wide range of variation on dimensions of interest. The diversity of participants increases the richness of the data received (Loiselle & ProfettoMcGrath, 2004). To ensure that the issues related to treatment decision making be as comprehensive as possible, two patient groups were invited to participate in the study. Patients who currently needed to make a treatment choice provided a prospective point of view. Patients who had already made a treatment choice provided a retrospective account of their experience and hindsight knowledge to describe the needs and gaps that would have facilitated their decision-making process.
The sample size was based on informational needs related to data saturation. Patients were recruited and interviewed until no new information was produced and redundancy was obtained. In this study, data saturation was achieved with nine participants. The two men and seven women ranged in age from 29 to 57 years and had been diagnosed with MS from 6 weeks to 9 years (Table 1). Participants spoke English or French. Three had secondary, five had postsecondary, and one had postgraduate education. All were Canadian born except one. Two were of Middle Eastern descent, and one was of Italian descent.
Procedure
Ethics approval for the study was obtained from the hospital research ethics committee. A study information pamphlet was created to briefly describe the study. Physicians and clinical nurse specialists in the MS program were invited to identify and contact potential candidates who met the study criteria and provided them with this information pamphlet. The pamphlets were also made available in the clinic waiting room so that patients could self-refer by contacting the researcher directly or indicate to the team that they agreed to be contacted. The researcher telephoned candidates who expressed an interest in the study. If the potential participant agreed to participate, written informed consent was obtained before the interviews began.
Data Collection
Participants were encouraged to talk about their decisionmaking experience during a 90- to 120-minute audiorecorded interview. At the discretion of each participant, the interviews took place at the participant’s homes or at the hospital. A semistructured interview guide was used to enable the participants to describe the experience from their own perspective and allowed the researcher to explore the relevance of certain factors for each participant’s situation. In keeping with the phenomenological approach, questions were purposefully exploratory and open-ended in structure so as to elicit rich descriptions without unduly imposing the assumptions and ideas held by the researcher. Given that the researcher had 10 years of experience in the field of MS and had been involved with the care of some participants, attempts were made to suspend (or bracket) preconceived beliefs or opinions regarding this experience for participants.
Interviews began with a broad question to encourage the telling of stories from the patient’s perspective. Further questions were posed to encourage expansion of their narrative and to elicit examples to illustrate this theme. Three participants (one each who had accepted, declined, or deferred treatment) were contacted a second time, after the analysis of data from their first interview, to validate the themes that the researcher was starting to develop.
The researcher gathered additional data from the health record for descriptive purposes and to provide a context from which to understand the experiences shared by the participants. These data included their age; gender; time since diagnosis; current medications; level of education; occupation; living arrangement; and expanded disability status score, a measurement of disability because of MS.
Data Analysis
After verbatim transcription of the interviews, Colaizzi’s (1978) seven procedural steps were used to analyze the data as follows:
a. Researcher read all transcribed narratives thoroughly to ensure the written text reflected the actual interview and to gain an understanding of participants’ experiences.
b. Significant statements that are related to treatment experiences were extracted and coded.
c. The transcribed data were analyzed and themes developed in the language in which the interview was conducted.
d. Statements were grouped according to the meanings that the researcher attributed to the statements.
e. Interpretations made to date were shared with three participants for review and validation of their individual experience (member checks).
f. Organization of the group formulated meanings into clusters of themes and categories.
g. Themes were integrated into a description of treatment decision making in individuals with MS.
Lincoln and Guba’s (1985) four criteria for establishing the trustworthiness of qualitative data were used in this study. Credibility or truthfulness of the data was enhanced by using more than one reviewer to analyze the data and provide peer debriefing. The process entailed independent review of the narratives and coding of responses, discussion of category, and theme development and consensus on the final coding of all responses of the participants (D.L. and J.R.). Dependability was confirmed by comparing the data analysis between the researcher and peer reviewer (D.L. and J.R.). Member checks with some of the participants served to provide feedback on the credibility of the data with confirmability addressed by returning to three participants to ensure the themes were congruent with their decision-making experiences. Transferability was related to the generalizability of data to other groups and was ensured by a broad sampling strategy to capture diverse participants’ experiences.
Findings
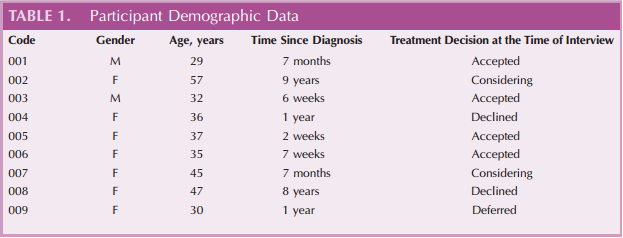
The nine participants in the study described decision making about treatment for their MS as part of a process of coming to a ‘‘redefined self.’’ Figure 1 conceptualizes the treatment decision-making experience and the themes that define that experience.
Core Theme: Redefined Self
In Figure 1, the inner circle contains the elements that made up the core theme of this study, a redefined self. The process of redefinition started with being diagnosed with MS and becoming a person with MS. Further deliberation occurred when participants were faced with treatment options, because they had to imagine themselves as a person on treatment. Thoughts about treatment hinged on reflections about their self-image (developmental, emotional, physical, and social), their life and career goals, and their present and future quality of life.
Themes Related to the Experience of Decision Making About Treatment
Six major themes were significant in the experience of decision making about treatment for MS. In Figure 1, these are represented as surrounding and providing support for the core theme of redefined self.
Weighing and Deciding What's Important
After receiving the diagnosis of MS, individuals described that they had engaged in a process of weighing what was important and considered different options when reflecting on the place of treatment in their life. Imagining life on treatment was part of the process of determining whether treatment was a way to achieve what they wanted or a threat to their sense of self. One participant said, ‘‘I had to visualize myself doing it and visualize accepting it before deciding on one. I wouldn’t have felt comfortable taking a treatment without pretending I was already taking one’’ (001). Another young woman shared her family’s struggles with the decisions they faced regarding the timing of medication initiation: ‘‘Any decision to do one thing that was different from the plan endangered something elseI. I was dealing with multiple variables, so I’d measure two against one another or this combination of choicesVschool, career, baby, and medication. Then I’d wait a couple of weeks and then I’d do another combination to see if anything changedI. We wanted to have children, it was just when. We said, ‘What are we gonna do? Is this the right order’?.... It was heart wrenching’’ (009).
Participants also weighed the information relating to the individual medications, while trying to reconcile the ambiguity and uncertainty related to the lack of clear benefit of one treatment over another. One person said, ‘‘so I went from wanting to choose the best medication to then realizingIthat they’re more or less equivalent and then really picking the one that would best fit with my lifestyle’’ (003). The commitment involved in starting the medication once the treatment decision was made was also identified as participants realized this was a lifelong therapy.
Acknowledging the Illness as Par of Oneself
After receiving the diagnosis, some participants readily acknowledged the illness as part of themselves, and their readiness to consider treatment followed. ‘‘I at least knew where I should be putting my mind, I have multiple sclerosis, let’s go!’’ (001). A number of participants had kept the illness hidden and were slowly acknowledging it was there. One woman had experienced anger and grief for 8 years since her diagnosis and had difficulty saying she had MS. She described, ‘‘accept it meansIit’s like if I would take the illness and say, ‘you are my friend’, or something like that. That’s not what I think. So I turn my back, and I say, ‘go away’!’’ (002). She had consistently declined treatment, but after experiencing a disabling attack, the option of treatment had been raised again. She struggled with having the previously hidden illness and treatment as part of her life, ‘‘It’s in the house, it’s part of me, but it’s still outside. It’s not in yetI. I’ll have to invite it inI’’ (002).
Another woman (007) considering treatment was relieved that her symptoms had ‘‘a name’’ but was just starting to consider herself as a person with MS when faced with a decision about treatment. Learning about treatment options also led to new discussions with her family about her illness.
Playing the Mental Game
Participants struggled with fear, uncertainty, and ambiguity of the illness and its treatment. One participant said, ‘‘It’s not the physical aspect of injection, it’s also the constant idea there is something wrong with me. It plays very much a mental game on your health as well, it’s like a black cloud’’ (003). Another young woman who had deferred treatment in favor of becoming pregnant shared, ‘‘It’s not just what is the best decision. Fear can really keep you from even exploring a problem’’ (009).
Seeking Credible Resources
Developing a strategy to learn about their illness and the available treatments was part of every participant’s story. Integral to this process was the seeking of opinions and lived experience of others with MS to assist them in the decisions they faced. ‘‘I wanted to go to people actually doing it, to look at their experiences. I wanted to make my own formulations based on who is doing well, who is not doing wellIand to make my own decision, based on what other people’s input is’’ (001). Another said, ‘‘What I was seeking at first was an unbiased forum in order to get this information,’’ referring to internet blogs on MS treatments (003). Another person reported, ‘‘I was afraid to see people in bad shape, who weren’t doing well, but finally I met someone and it was good for me (to help decide to start treatment). She was there at the right time’’ (006, translated from French). A number of participants shared that the opinions of their peers were the most credible source of information related to treatment.
Evaluating Symptoms and Fit With Quality of Life
A turning point for decision making about treatment revolved around the participants’ perception of disability related to MS. Some participants could anticipate E18 Journal of Neuroscience Nursing Copyright © 2014 American Association of Neuroscience Nurses. Unauthorized reproduction of this article is prohibited. they might develop disability with MS and took a proactive approach, readily embracing the notion of treatment. For others, real or anticipated symptoms were not enough to tip the balance in favor of starting therapy. Only when the symptoms affected function and quality of life, or interfered with the achievement of valued goals or threatened self-image, did participants in this study consider treatment. An individual who had declined treatment for many years and had experienced a severe, disabling relapse reported, ‘‘Things were stable, that’s why I didn’t want to take anythingIno treatments (emphasis added), but I said, ‘maybe if I can try a treatment so that it will just put aside my relapses that will be ok’. You know, to gain my life back’’ (002).
Others continued to decline treatment when offered despite numerous relapses and daily symptoms. One participant was sceptical of the benefits of treatment and possible side effects: ‘‘It’s been a long time that I haven’t had a relapse. I say I didn’t have a relapse because I stopped work, I decreased my stress level, I managed my energy and I dealt with my illness.’’ She acknowledged that she had daily symptoms: ‘‘There are things that have persisted, like my fatigueI. it needs to be managed each day. Every day there are things that I cannot do’’ (008). Another young woman who had declined treatment and opted to try lifestyle modifications to manage her illness could anticipate a time when she might reconsider: ‘‘If I had like my feet dragging on the floor, if I was paralyzedI. I think maybe then I would say, ‘I’m going to give it a chance.’ It’s difficult to decide, but for now I feel good’’ (004).
Managing Roles and Involvement of Family
Family members provided support, encouragement, and often, filtered information about MS and its treatments when the participant was trying to cope with the treatment decision. Some participants described working as a team with their family around the notion of treatment but ultimately made their own decision about how to proceed. Another participant, making a decision about treatment at the time of our interview, discussed how being offered treatment challenged some of her coping strategies. Before this, she had avoided learning about the illness and treatment and had kept the diagnosis hidden from her family. An upcoming clinic visit prompted her to review a DVD on treatment choices and initiate the discussion with her family about her illness. ‘‘I waited to tell themI. it was kind of like hidden. I had put the treatment information away. I didn’t want them to see it’’ (007). In some cases, a family member’s decision-making style was perceived as being incongruent with that of the person with MS. ‘‘My mom wasn’t even considered in it.... she’s really not reliable. She just thinks with her heart, more than with her mind’’ (001).
The Context of Treatment Decision Making
Although the six themes formed the core of the treatment decision-making experience, participants discussed other perceptions, beliefs, and issues that provided the context for the choices they made regarding treatment. This context is represented in the outer circle of Figure 1.
Social Construction of Illness
Once diagnosed with MS, participants reflected on the place of their illness in a broader social context, sometimes identifying MS as a stigma. One person said, ‘‘A cancer would be ok; that you can talk about. People are so close to cancer, but MS they are not’’ (002). Another suggested with respect to medications, ‘‘everyone takes pills, everyone knows pills and that’s normal. Taking an injection is not normal’’ (007).
Previous Experiences With Illness and Treatment
Previous experiences and beliefs regarding illness and treatment also came into play when participants made decisions about their own therapy. The need to take a treatment was normalized for several participants if family members or friends already took some type of medication, particularly by injection. One said, ‘‘I know MS is just one of several diseases, like my father is diabetic and he takes a needle for thatIso people have to do these things’’ (001). One young woman who had declined treatment reflected on her sister’s diabetes: ‘‘I just think that sometimes diabetes ‘defines her’ and obviously because she is taking insulin, I cannot switch off from forgetting that she’s got diabetesIwhich is a big part of her life. For me, MS is still not a big part of my life’’ (004). None of the participants in this study identified fear of injections as an influence on whether to start treatment.
Timing of Decision Making
The amount of time elapsed since diagnosis was an important issue related to decision-making discussion. Participants felt ill-equipped to make treatment decisions early in the illness trajectory. One reported, ‘‘I was offered the possibility of getting a treatment, but I only had something like 24 hours to decideIand I said, ‘forget it,’ I need to learn more about it ’’ (003). Another said, ‘‘It was slightly overwhelming. My physician said, you can choose between medication x, y, and zI. I had no knowledge of the disease and it was a lot, because I didn’t even understand what was wrong with me’’ (005). Being told that they could make the decision about which medication to take felt overwhelming and strange for some participants. One person said, ‘‘It was a definite paradigm shift for me, picking my medication. It’s kind of like picking your own poison in some waysI’’ (003). This participant, along with others who expressed an initial hesitancy, wanted to take a more active role in their treatment choice after having time to learn about the illness and the treatment options available.
Relationship With Healthcare Practitioners
All participants reflected on their relationships with healthcare providers around treatment issues and the ‘‘goodness of fit’’ between their decision-making styles as well as the congruence regarding whether to go on treatment. One participant chose her physician based on the one that agreed with her philosophy on treatment: ‘‘What I like about him was that even though he prescribes conventional medicine, he also believes in the mental power of thingsIso (he didn’t) take hope away from you’’ (004).
Access to Information
All participants sought accurate information about the illness and its treatment using a variety of sources. One reported, ‘‘When you have no information it’s awful, you really, really worry and you expect the worst’’ (005). Some shared the challenges of becoming informed. One reported, ‘‘sometimes its too much informationIyou can go in all different directions’’ (007).
Support for Decisions to be Made
Participants reported that, in addition to having access to information about MS therapies, they needed someone to help them with decision making about treatment. One individual reported, ‘‘You’re never going to come to a decision on your ownI. you really need a person too who can ask, what are the issues in your life, what are you facing right now?’’ (009) A number of participants turned to their nurse as a source of unbiased information and reported that the nurse made things more ‘‘tangible’’ and helped to solidify their decision. One participant who did not have access to a nurse during the treatment decision process identified this as a significant gap in her care.
The Process of Decision Making About Treatment for MS
As we examined how the themes unfolded, it became clear that the participants, regardless of their decision to accept or not accept treatment, had taken similar steps in their decision-making process that were central to the appropriateness of support interventions (Figure 2). Although the process appears to be sequential, the process was more iterative, than linear, allowing participants to reflect on new information and thoughts as they arose.
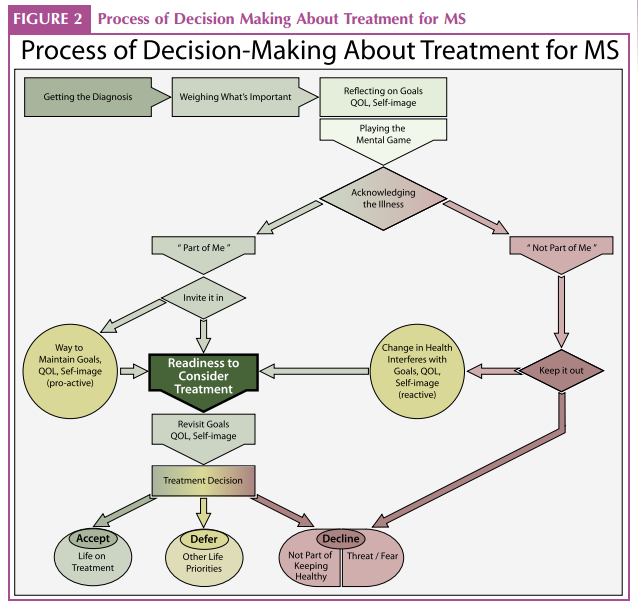 Receiving a diagnosis of MS resulted in feelings of fear, uncertainty, and sometimes, relief that the diagnosis was not worse. Some participants described gathering information about MS and its treatment from the healthcare team, various online sources, and the lived experience of others with MS. Others avoided information about the disease and its evolution over time. Beliefs about the diagnosis of MS and family experiences with illness were brought in as they weighed what was important in relation to their goals, quality of life, and self-image. Relapses and currently experienced symptoms influenced the degree to which the illness represented an intrusion and threat to their current and future life. Some participants readily acknowledged they had the illness, whereas others reported keeping it private. Those who had ‘‘invited the illness in’’ were, in many cases, ready to reflect on treatment as a way to maintain a life they valued. Those who had kept the illness ‘‘out’’ demonstrated a reluctance to consider treatment. It was when they perceived that the illness threatened their quality of life, goals, and self-image that they reconsidered their treatment options.
Receiving a diagnosis of MS resulted in feelings of fear, uncertainty, and sometimes, relief that the diagnosis was not worse. Some participants described gathering information about MS and its treatment from the healthcare team, various online sources, and the lived experience of others with MS. Others avoided information about the disease and its evolution over time. Beliefs about the diagnosis of MS and family experiences with illness were brought in as they weighed what was important in relation to their goals, quality of life, and self-image. Relapses and currently experienced symptoms influenced the degree to which the illness represented an intrusion and threat to their current and future life. Some participants readily acknowledged they had the illness, whereas others reported keeping it private. Those who had ‘‘invited the illness in’’ were, in many cases, ready to reflect on treatment as a way to maintain a life they valued. Those who had kept the illness ‘‘out’’ demonstrated a reluctance to consider treatment. It was when they perceived that the illness threatened their quality of life, goals, and self-image that they reconsidered their treatment options.
Whether initially accepting treatment or reconsidering treatment after declining, a reappraisal seemed to occur during which individuals imagined life on treatment, considered options related to timing and treatment type, and gathered information and experiences of others to help them reach a decision. The decision to start a treatment was influenced by the perception that treatment was a way to maintain or achieve objectives they valued. In one case, an individual who decided on treatment deferred treatment again in favor of another life priority, pregnancy. Some participants declined treatment or delayed treatment decision making out of fear of facing the illnessVthe treatment symbolized a constant, daily reminder of their disease. Two individuals refused treatment because they did not feel that treatment was part of what kept them healthy. They accepted having a diagnosis of MS, had adequate information about the illness and the benefits and risks of treatment or nontreatment, and may or may not have had difficult symptoms to deal with. Whether they were disabled at the time of the interviews, they did not experience the disease or its sequelae as a threat and actively chose to not pursue treatment.
Discussion
The findings of this study describe treatment decision making for MS to be inextricably woven in the experience of the illness itself. Most of the participants had been diagnosed for less than a year and recounted that the newness of living with MS was still very much in the foreground of their daily lives. Reconciling the uncertainty of treatment benefit while adjusting to the diagnosis was a challenge for many in this study. The core theme of ‘‘redefining self’’ presents an important aspect to consider in the iterative process involved in making a decision about treatment for MS; individuals would not consider treatment until this redefinition of self was done. In addition, there was a lack of a unidirectional process through the decision-making steps, suggesting that decision making is not always a linear process. These findings have important implications for practices related to supporting decision making about treatment.
The finding that the treatment decision-making experience entailed a process of redefining self supports other researchers’ findings that the sense of self changes after being diagnosed with MS (Dennison, Yardley, Devereux, & Ross-Morris, 2010; Mozo-Dutton, Simpson, & Boot, 2012) or HIV (Baumgartner & David, 2009). The process of weighing described by the participants is consistent with Isaksson and Ahlstro¨m’s (2006) report that patients with MS balance acknowledging and fighting the disease with ‘‘backward and forward’’ movement during the adjustment stages. For our participants, symptoms alone did not influence the decision to accept treatment until those symptoms affected perceived quality of life or threatened their sense of self. At that point, the participants revisited their goals, quality of life, and self-image and reconsidered taking a treatment. Mozo-Dutton et al. also found that treatments were considered only when MS symptoms had an impact on a person’s ability to fulfill valued roles that the sense of self was called into question. For our participants, choosing a treatment meant acknowledging the diagnosis, picturing themselves as someone with MS, and imagining being on treatment. Similarly, Baumgartner and David reported that a ‘‘turning point’’ occurred for those with HIV upon the realization of the need to take medication for their condition.
Many participants described not being ready to make treatment decisions soon after their diagnosis. Dennison et al. (2010) and Isaksson et al. (2006) reported concerns about the challenges of decision making when the diagnosis is new and overwhelming. The participants also described the additional challenge raised by the nature of MS pharmacotherapies and the variation related to individual and disease situations (Fazekas et al., 2010; Freedman et al., 2004). Our participants found these areas of uncertainty to be stressful and that the stress was compounded by some of the healthcare providers’ approaches. Ziebland, Evans, and McPherson (2006) and Elit et al. (2002) reported similar responses in patients with ovarian cancer when there was not a clear treatment choice.
Our participants varied in the extent to which they moved to the stage of acknowledging that they had MS and required treatment. They not only wanted comprehensive information about choices but also valued the lived experience and ‘‘peer evidence’’ of others on treatment. Similarly, Ziebland et al. (2006) reported that ovarian cancer patients wanted to see, hear, and read about the real experiences of others.
Our study findings raise important questions about the appropriate timing of discussions about treatment and use of such interventions as decision aids. For instance, those participants who had not yet reached the point of considering MS as part of their identity were unwilling to receive information, education, or decision support relating to disease-modifying therapies. Some reevaluated earlier treatment decisions only when they experienced new illness-related events, even many years after diagnosis. At that point, there was an opportunity to introduce decision support and decision aids. Use of such decision aids, therefore, may be premature for those in the MS populations not yet ready to do such deliberative work.
Implications
Our study findings have many implications for nurses and other healthcare practitioners involved in facilitating the treatment decision-making process of patients with MS. Most importantly, nurses need to assess the patient’s readiness to engage in a discussion about treatment soon after diagnosis, a time when they may feel vulnerable and may be experiencing emotional distress (Isaksson, 2006). Patients may need time to make sense of the diagnosis and to understand what it may mean for them and their families, before deciding on whether to take a treatment. Asking questions about how they perceive their diagnosis and what it means to have this illness may give insights into whether they have incorporated the illness as part of their identity and whether they might be receptive to incorporating a treatment as part of their lives.
The results also illustrate that making a decision about treatment for MS is more complex than a straightforward, linear process of gathering knowledge of MS and its treatments and then choosing among several therapies. Although it is important for patients to receive education about different treatment alternatives (Denis et al., 2004; Keating & Ostby, 1996), there is also a need to explore the values, beliefs, and expectations related to the treatment and not, as KellyPowell (1997) notes, just to focus on the statistical effectiveness of the therapy. Nurses need to appreciate that being invited to make a treatment choice early in the phase after diagnosis may seem inappropriate and untimely as individuals with ovarian cancer have reported (Ziebland et al., 2006). The teaching process should include information on why patients may be offered a choice among several therapies and the clinical uncertainty about the one best treatment for them at the outset. Checking with patients about the degree of decision-making control they desire and then responding to that preference may help allay the stress of assuming responsibility for a treatment decision and reduce the fear of making the wrong choice (Degner & Sloan, 1997). Our study illustrated that the desired degree of decision-making involvement changed over time as patients felt more competent in managing their disease, suggesting that treatment decision control preferences should be reevaluated at different junctures along the illness trajectory rather than at one time point (Giordano et al., 2008).
For those ready to engage in discussions about treatment, nurses can provide information, clinical counseling, decision tools, and coaching to patients and their families so they can make informed, values-based decisions (O’Connor, Jacobsen, & Stacey, 2002). Recognizing that patients value the lived experience of others, nurses can guide patients to support groups or Web sites that may enable them to connect with their peers. New illness-related events such as relapses of the disease provide an opening to revisit a previous treatment decision, especially if patients express that there has been a negative impact on their quality of life. Nurses can use this opportunity to explore readiness to reconsider treatment, to reeducate about MS and available therapies, and introduce tools such as decision aids to facilitate a decision choice.
Limitations
Limitations in this study include the small sample size, although saturation of themes was achieved (Sandelowski, 1995). Responders to the advertisements about the study may have been more willing to discuss their experiences than nonresponders. The views of the participants of this study represent those attending a large, university teaching hospital MS clinic and may not be representative of all patients with relapsing-remitting MS. Finally, the treatment landscape in MS is changing rapidly, and patients may face different issues in the future as they make decisions about treatment for their disease.
Conclusions
This study makes a contribution to the treatment decision-making dimension of the patient experience of living with MS. Redefining self as a person with MS preceded the readiness to consider treatment. A complex and iterative process followed in which patients reflected on the place of treatment in their lives. Nurses can use this knowledge to engage and partner with patients as they decide if and when to invite disease-modifying therapies for MS into their lives.
Acknowledgements
This study was supported by a grant from the Eureka! Fellowship in Nursing Research at the McGill University Health Centre funded by Richard and Satoko Ingram of the Newton Foundation and the Foundations of the Royal Victoria, Montreal General, and Montreal Children’s Hospitals. The study was also supported by a grant from the Canadian Nurses Foundation.
References
Barker-Collo, S., Cartwright, C., & Read, J. (2006). Into the unknown: The experiences of individuals living with multiple sclerosis. Journal of Neuroscience Nursing, 38(6), 435.
Baumgartner, L. M., & David, K. N. (2009). Accepting being poz: The incorporation of the HIV identity into the self. Qualitative Health Research, 19(12), 1730Y1743.
Berger B. A., Hudmon, K. S., & Liang, H. (2004). Predicting treatment discontinuation among patients with multiple sclerosis: Application of a transtheoretical model of change. Journal of American Pharmacists Association, 44(4), 445Y454.
Carder, P. C., Vuckovic, N., & Green, C. A. ( 2003). Negotiating medications: Patient perceptions of long-term medication use. Journal of Clinical Pharmacy and Therapeutics, 28(5), 409Y417.
Colaizzi, P. (1978). Psychological research as the phenomenologist views it. In R. Valle & M. King (Eds.), Existential phenomenological alternatives for psychology. New York, NY: Oxford University Press.
Degner, L., & Sloan, J. (1997). The control preferences scale. Canadian Journal of Nursing Research, 29, 21Y43.
Denis, L., Namey, M., Costello, K., Frenette, J., Gagnon, N., Harris, C., I Poirier, J. (2004). Long-term treatment optimization in individuals with multiple sclerosis using disease-modifying therapies: A nursing approach. Journal of Neuroscience Nursing, 36(1), 10Y22.
Dennison, L., Yardley, L., Devereux, A., & Moss-Morris, R. (2010). Experiences of adjusting to early stage multiple sclerosis. Journal of Health Psychology, 16(3), 478Y488.
Derwenskus, J. (2011). Current disease modifying treatment of multiple sclerosis. Mount Sinai Journal of Medicine, 78, 161Y175.
Elit, L., Charles, C., Gold, I., Gafni, A., Farrell, S., Tedford, S., I Whelan, T. (2002). Women’s perceptions about treatment decision-making for ovarian cancer.Gynecologic Oncology, 88, 89Y95.
Fazekas, F., Baumhackl, U., Berger, T., Deisenhammer, F., Fuchs, S., Kristoferitsch, W., I Vass, K. (2010). Decision making for and impact of early immunomodulatory treatment: The Austrian Clinically Isolated Syndrome Study (ACISS). European Journal of Neurology, 17(6), 852Y860.
Fraser, C., Hadjimichael, O., & Vollmer, T. (2001). Predictors of adherence to Copaxone therapy in individuals with relapsingremitting multiple sclerosis. Journal of Neuroscience Nursing, 33(5), 231Y239.
Freedman, M. S., Patry, D. G., Grand’Maison, F., Myles, M. L., Paty, D. W., & Selchen, D. H.; Canadian MS Working Group. (2004). Treatment optimization in multiple sclerosis. Canadian Journal of Neurological Sciences, 31(2), 157Y168.
Gasperini, C., & Ruggieri, S. (2011). Emergine oral drugs for relapsing-remitting multiple sclerosis. Expert Opinion on Emerging Drugs, 16(4), 692Y712.
Giordano, A., Mattarozzi, K., Pucci, E., Leone, M., Casini, F., Collimedaglia, L., & Solari, A. (2008). Participation in medical decision-making: Attitudes of Italians with multiple sclerosis. Journal of the Neurological Sciences, 275, 86Y91. Giovannoni, G., Southam, E., & Waubant, E. (2012). Systematic review of disease-modifying therapies to assess unmet needs in multiple sclerosis: Tolerability and adherence. Multiple Sclerosis Journal, 18(7), 932Y946.
Goodin, D. S., Frohman, E. M., Garmany, G. P. Jr., Halper, J., Likosky, W. H., Lublin, F. D., I van den Noort, S. (2002). Disease-modifying therapies in multiple sclerosis: Subcommittee of the American Academy of Neurology and the MS Council for Clinical Practice Guidelines. Neurology, 58, 169Y178.
Heesen, C., Ko¨pke, S., Richter, T., & Kasper, J. (2007). Shared decision-making and self-management in multiple sclerosisVA consequence of evidence. Journal of Neurology, 254(Suppl 2), II/116YII/121.
Heesen C., Solari A., Giordano A., Kasper J., & Ko¨pke S. (2011). Decisions on multiple sclerosis immunotherapy: New treatment complexities urge patient engagement. Journal of the Neurological Sciences, 306, 192Y197.
Isaksson, A.-K., & Ahlstro¨m, G. (2006). From symptoms to diagnosis: Illness experiences of multiple sclerosis patients. Journal of Neuroscience Nursing, 38(4), 229Y237.
Keating, M. M., & Ostby, P. L. (1996). Education and selfmanagement of interferon beta-1b therapy for multiple sclerosis. Journal of Neuroscience Nursing, 28(6), 350-2, 357-8.
Kelly-Powell, M. L. (1997). Personalizing choices: Patients’ experiences with making treatment decisions. Research in Nursing & Health, 20, 219Y227.
Lincoln, Y. S., & Guba, E. G. (1985). Naturalistic inquiry. Newbury Park, CA: Sage.
Loiselle, C., & Profetto-McGrath, J. (2004). Canadian essentials of nursing research. Philadelphia, PA: LippincottWilliams &Wilkins.
Markowitz, C. E. (2010). The current landscape and unmet needs in multiple sclerosis. American Journal of Managed Care, 16(Suppl 8), S211Y218.
Morgante, L., Hartley, G., Lowden, D., Namey, M., LaRocca, T., & Shilling, J. (2006). Decision-making in multiple sclerosisV From theory to practice. International Journal of Multiple Sclerosis Care, 8, 113Y120.
Mozo-Dutton, L., Simpson, J., & Boot, J. (2012). MS and me: Exploring the impact of multiple sclerosis on perceptions of self. Disability and Rehabilitation, 34(14), 1208Y1217.
O’Connor, A. M., Bennett, C. L., Stacey, D., Barry, M., Col, N. F., Eden, K. B., I Rovner, D. (2009). Decision aids for people facing health treatment or screening decisions. Cochrane Database of Systematic Reviews, 3, CD001431.
O’Connor, A. M., Jacobsen, M. J., & Stacey, D. (2002). An evidence-based approach to managing women’s decisional conflict. Journal of Obstetric, Gynecologic, & Neonatal Nursing, 31(5), 570Y581.
Saida, S., Eckstein, C., & Calabresi, P. (2012). New and emerging disease modifying therapies for multiple sclerosis. Annals of the New York Academy of Sciences, 1247, 117Y137.
Sandelowski, M. (1995). Focus on qualitative methods: Sample size in qualitative research. Research in Nursing and Health, 18(2), 179Y183.
Scalfari, A., Neuhaus, A., Degenhardt, A., Rice, G. P., Muraro, P. A., Daumer, M., & Ebers, G. C. (2010). The natural history of multiple sclerosis, a geographical based study 10: Relapses and long-term disability. Brain, 133, 1914Y1929.
Smeltzer, S. (2002). Reproductive decision-making in women with multiple sclerosis. Journal of Neuroscience Nursing, 34(3), 145Y158.
Solari, A., Martinelli, V., Trojano, M., Lugaresi, A., Granella, F., Giordano, A., I Borreani, C. (2010). An information aid for newly diagnosed multiple sclerosis patients improves disease knowledge and satisfaction with care. Multiple Sclerosis, 16(1), 1393Y1405.
Stacey, D., Bennett, C. L., Barry, M. J., Col, N. F., Eden, K. B., Holmes-Rovner, M., & Llewellyn-Thomas, H. L. (2012). Decision aids for people facing health treatment or screening decisions (review): The Cochrane Collaboration. West Sussex, England: Wiley.
Stacey, D., Kryworuchko, J., Bennett, C., Murray, M., Mullan, S., & Legare, F. (2012). Decision coaching to prepare patients for making health decision: A systematic review of decision coaching in trials of patient decision aids. Medical Decision Making, 32, E22YE33.
Thorne, S., Con, A., McGuinness, L., McPherson, G., & Harris, S. R. (2004). Health care communication issues in multiple sclerosis: An interpretive description. Qualitative Health Research, 14, 5Y22.
Thorne, S., Paterson, B., & Russell, C. (2003). The structure of everyday self-care decision making in chronic illness. Qualitative Health Research, 13(10), 1337Y1352.
Wagner, E. H. (1998). Chronic disease management: What will it take to improve care for chronic illness? Effective Clinical Practice, 1, 2Y4.
Ziebland, S., Evans, J., & McPherson, A. (2006). The choice is yours? How women with ovarian cancer make sense of treatment choices. Patient Education and Counseling, 62, 361Y367.